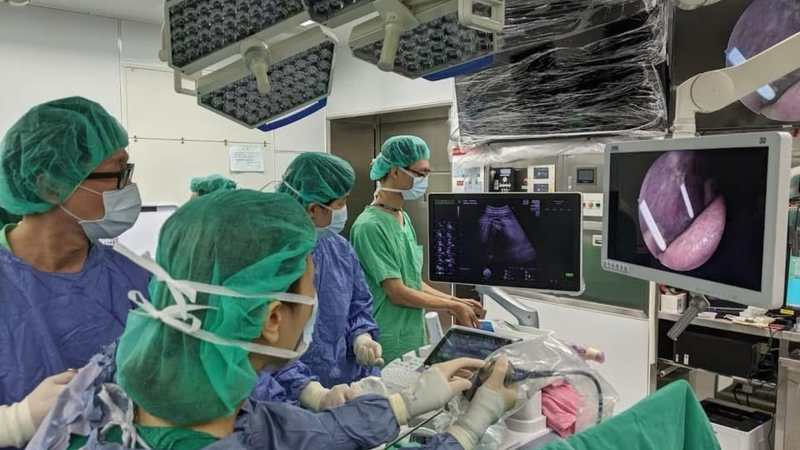
At 23 weeks of pregnancy, Ms. Lu’s fetus was diagnosed with myelomeningocele, a condition that left her baby facing a lifetime of paralysis after birth. Struggling with the agonizing decision, Ms. Lu initially planned to terminate the pregnancy. However, after transferring to Taipei Chang Gung Memorial Hospital and having multiple in-depth discussions with Dr. Steven Shaw, she decided to undergo a "Fetoscopic Spinal bifida Repair" to give her baby a chance at life. The surgery was performed in 2021. Today, the little girl is four and half year-old. Her lower limb motor function is completely normal; she can run and jump naturally and does not require a ventriculoperitoneal (VP) shunt. She only needs regular follow-ups. This milestone sets a new record for fetal therapy in Taiwan. Doctors urge expectant parents not to despair over abnormal prenatal diagnoses, as minimally invasive surgery offers a new choice for life.
Myelomeningocele Causes Severe Fetal Nerve Damage
Professor Jie-Tsai Wu of the Department of Neurosurgery at Linkou Chang Gung Memorial Hospital pointed out that myelomeningocele (MMC) is the most severe form of spina bifida, with an incidence rate of approximately 1.87 per 10,000 births in Taiwan. In these fetuses, the spinal nerves are directly exposed to the amniotic fluid. As the pregnancy progresses, the chemical composition of the amniotic fluid causes irreversible toxic damage to the nerves, leading to postnatal lower limb paralysis, bowel and bladder incontinence, and even severe hydrocephalus and Arnold-Chiari malformation.
Introducing Brazilian Technology: Minimally Invasive "Three-Hole" Surgery Saves a Life
Dr. Steven Shaw, Director of the Department of Obstetrics and Gynecology at Taipei Chang Gung Memorial Hospital, stated that the surgical technique used in this case originated in Brazil. Utilizing the minimally invasive fetoscopic surgery, the medical team made only three puncture holes in the pregnant woman's abdomen and uterus. Carbon dioxide was used to expand the amniotic cavity to insert the endoscope and delicate surgical instruments. During the repair process, doctors must operate in a highly confined space, covering the exposed spinal nerves with a special "biocellulose patch" and suturing it in place. In contrast, traditional "open fetal surgery" requires a large incision in the mother's abdomen and uterus, which carries high risks, may lead to premature birth or uterine rupture, and restricts future deliveries to Cesarean sections only.
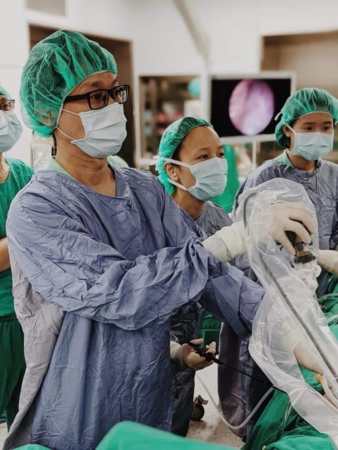
(Photo by Chang Gung Memorial Hospital)
Dr. Ya-Chun Chuang, an attending physician at Taipei Chang Gung's OB/GYN, noted that the mother in this successful case received the abnormal fetal diagnosis at 23 weeks and underwent surgery at 27 weeks. The procedure took only 126 minutes with minimal blood loss. The baby was born at 32 weeks, weighing 2,295 grams. Professor Wu mentioned that following the prenatal skin coverage, the newborn underwent a postnatal neurosurgical repair and has an excellent prognosis. Professor Chin-Man Wang of Pediatric Rehabilitation at Linkou Chang Gung pointed out that the child's rehabilitation case was officially closed at around one year of age; she currently requires no rehabilitation therapy and only needs regular follow-ups.
Cross-Department Collaboration Lights the Beacon of Hope
Dr. Liang-Ming Lo, Vice Superintendent of Taipei Chang Gung Memorial Hospital, stated that the successful completion of this rare "fetoscopic spina bifida repair" in Taiwan is attributed to robust multidisciplinary team collaboration. Members included experts from Taipei Chang Gung's OB/GYN, and Linkou Chang Gung's Neurosurgery, Neonatology, Pediatric Rehabilitation, and Pediatric Nephrology departments.
The Dilemma: A Staggering 93% Termination Rate
Ms. Lu shared her feelings from that time, saying, "Back then, this technology was not yet mature in Taiwan and was part of a new medical technology project under the Ministry of Health and Welfare. I was extremely worried about the 'fate' my baby would face after birth, so I had decided to terminate the pregnancy. But after meeting Dr. Shaw and discussing it with him multiple times, I decided to give it a try and give my daughter a chance."
Director Shaw expressed, "Although our surgical techniques are fully in place, the research team witnessed the profound helplessness of Taiwanese society during the promotion process." He noted that this clinical trial, approved by the Ministry of Health and Welfare, recruited 15 families diagnosed with fetal spina bifida between 2020 and 2023. The team provided comprehensive interdisciplinary counseling involving pediatric neurosurgeons, neonatologists, and obstetricians to detail the treatment options. However, 14 families (a staggering 93%) ultimately chose to terminate the pregnancy between 18 and 26 weeks.
Three Main Reasons Behind the High Termination Rate for MMC
The Chang Gung research team believes the reasons behind the high termination rate are complex, primarily consisting of three factors:
- Fear of the future: Parents worry about the risk of their child remaining disabled after birth, as a 100% cure cannot be guaranteed.
- Economic and caregiving pressure: The long-term costs of rehabilitation and the immense human effort required for caregiving represent a heavy burden.
- Socio-cultural factors: The intense pressure from traditional Asian family values and the lack of a comprehensive social support system.
Director Shaw noted that compared to a fetal surgery acceptance rate of about 40% to 60% in Western countries, Taiwan and other Asian nations generally face extremely high termination rates. He sighed, "This is an incredibly difficult decision. We understand the parents' anxiety, but it also highlights the urgent need for broader societal education."
Don't Despair Over Abnormal Prenatal Diagnoses: Minimally Invasive Surgery Offers New Choices
The Chang Gung research team emphasized that this successful case shatters the fate of children with spina bifida being "either paralyzed or disabled" and proves that "spina bifida is not a terminal illness." Fetoscopic surgery can significantly improve a child's prognosis, giving them the opportunity to walk and attend school like normal children. Chang Gung Memorial Hospital hopes that by sharing these achievements, public awareness of fetal therapy will be elevated, ensuring that future expectant parents facing abnormal prenatal diagnoses will no longer see "giving up" as their only option, but can instead embrace the dawn of "treatment."

(Photo by Chang Gung Memorial Hospital)